A common misnomer about hypomania is that it is a mental illness like schizophrenia.
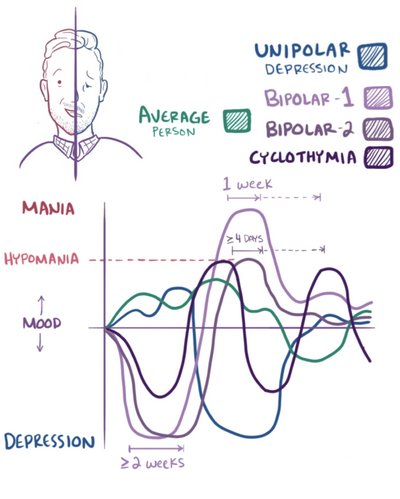
This is false, and it is often used to refer to bipolar affective disorder (BAD), another common misnomer. While it is true that some people are simply not capable of understanding the difference between a bipolar disorder and hypomania, many people with bipolar disorder also suffer from hypomania, which can have severe consequences. In this article, we will discuss hypomania and its relationship to bipolar disorders in general.
A. A hypomanic episode is usually characterized by a heightened feeling of euphoria, usually lasting for just a few days or weeks. It is more commonly described as an energy state, not unlike hypnosis, but more intense than that, and not easily equated with depression.
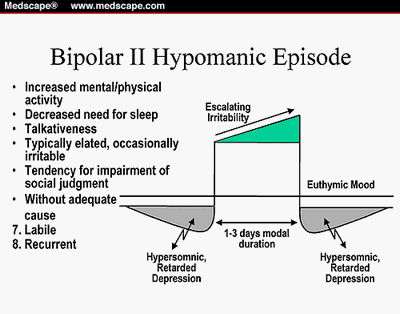
The term hypomanic sometimes tends to conflate some people, due to the “hyp” suffix. However, a true hypomanic is not a manic-depressive disorder, but rather a bipolar depressive syndrome (BD/HD) that occurs under the influence of hypomania, and may in turn lead to another psychiatric condition.
B. When hypomania is related to depression, it can be difficult to distinguish from normal behavior. Hypomanic episodes often involve an urge to escape or a need to feel “special,” but are not necessarily accompanied by an increase in mood, anger, agitation, suicidal thoughts, or hallucinations. When depressed, hypomanic symptoms are often mistaken as the symptoms of depression, and the patient may even believe that they are experiencing symptoms of depression, when in fact they are not. For this reason, hypomania can often present as normal mood swings, as well as being triggered by certain stimuli.

This can be a problem for sufferers, as it makes their treatment difficult.
C. Some research has found that hypomania can actually increase the risk of developing bipolar disorder in adults. This may be attributed in part to the increased risk of bipolar depression during childhood, and in part to a genetic disposition toward bipolar disorder. In either case, however, hypomania has been linked to high suicide rates, and is known to play a role in suicide attempts.
D. Many people with bipolar disorder suffer from hypomania.
A few studies suggest that people who suffer from bipolar disorder and hypomania are at greater risk for bipolar suicide attempts.
E. The most obvious connection between hypomania and bipolar disorder is that the two disorders are often co-occurring. People with one disorder often have a low or undetectable amount of hypomania. When it increases, the symptoms of the other disorder may occur as well, causing severe problems for the sufferer. This can result in an increased risk of suicide attempts and an increased likelihood of depression in those already suffering from depression.
F. Hypomania occurs as a symptom of depression, and is often a sign that a patient has a potentially dangerous condition.
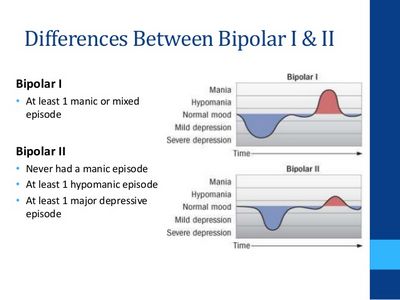
Research on hypomania and depression suggests that hypomania can lead to an increased risk of suicide attempts. In some cases, the cause of hypomania and depression may be the same, with the patient displaying symptoms of both conditions together, making it difficult to treat and diagnose depression and hypomania separately. However, most researchers believe that hypomania, or at least one component of it, is caused by the other, resulting in the need for a combination of treatment, including medication.
G. It is important to note that hypomania may be related to bipolar disorder, but not necessarily. It has also been linked to many types of mental illnesses, and is commonly a symptom of depression in many patients. Those who are concerned about possible side effects of prescription medications should seek out a medical professional who specializes in this area.